A single missing code, outdated insurance record, or incomplete document can stop a claim from being paid. Across the United States, nearly 30% of healthcare claims are denied or rejected on their first submission, costing providers billions each year (MGMA Cost and Revenue Survey, 2024).
Medical billing services exist to prevent exactly that. They are the financial foundation of every healthcare practice, ensuring providers get paid correctly, claims stay compliant, and revenue keeps moving.
This guide provides a comprehensive view of medical billing, including processes, what types of services exist, common challenges, where technology is heading, and why outsourcing makes more sense than most practices realize.
What is Medical Billing?
Medical billing is the process of translating healthcare services into claims submitted to insurers and following up to ensure payment.
Each claim represents a patient’s visit, including their diagnosis, the care provided, and the procedures performed, all translated into standardized codes that insurers recognize.
Effective billing depends on a clear understanding of:
- ICD-10, CPT, and HCPCS coding systems
- Payer-specific rules and documentation requirements
- HIPAA and CMS compliance standards
Even small errors can be costly. For example, coding Type 2 diabetes as Type 1 (E10.9 instead of E11.9) can result in a denial and delayed reimbursement. Accuracy and attention to detail ensure providers are paid in full and on time.
Medical Billing vs Medical Coding
These terms are often used together but they are not the same thing. Here is a simple way to think about it.
Coding converts the clinical note into standard codes. Billing takes those codes and turns them into claims, then follows up until the money is posted. If a coder assigns CPT 99213 for an office visit and ICD-10 E11.9 for Type 2 diabetes, the biller uses those codes to create the claim, submit it, and handle appeals if needed. An error at either step can slow or stop payment.
Medical Billing vs Coding Functions
| Function | Coding | Billing |
|---|---|---|
| Purpose | Convert services into standardized codes | Create claims and track payment |
| Responsibility | Certified coders | Billers or billing specialists |
| Outcome | Accuracy in documentation | Timely reimbursement |
Medical Billing Process Steps: The Complete Revenue Cycle Explained
The medical billing process, often called the revenue cycle, is a multi-step journey that starts before the patient sees the doctor and ends long after they have left. Each step is crucial for ensuring claim accuracy and prompt payment.
The 7 Steps of the Medical Billing Cycle
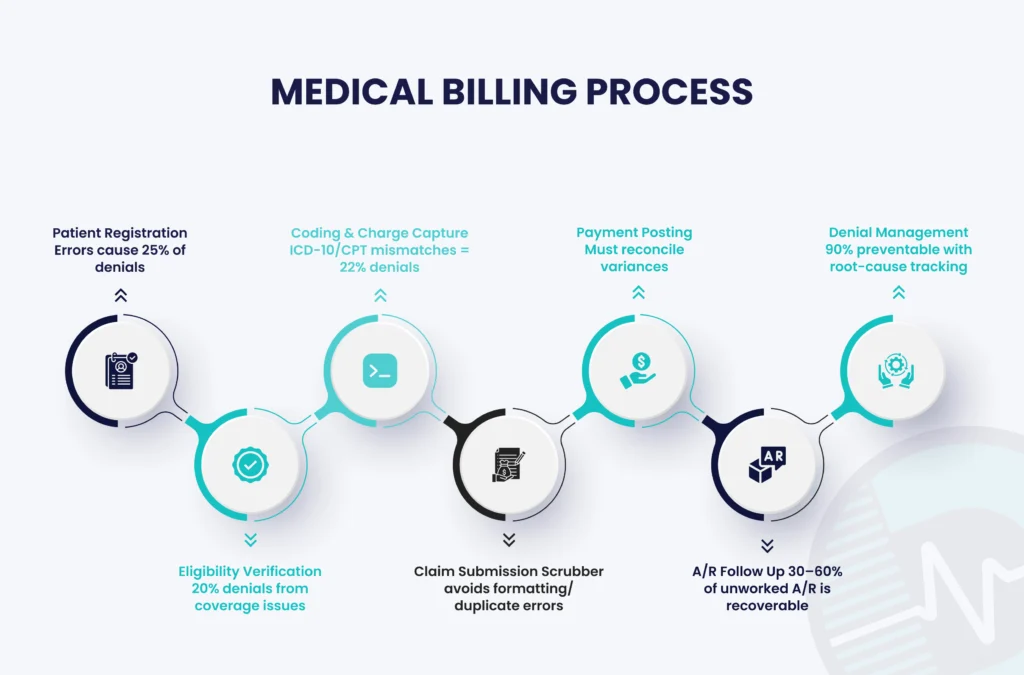
| Step | Description | Purpose and Impact |
|---|---|---|
| 1 | Patient Registration & Insurance Verification | Gather accurate demographic info and verify insurance status to avoid future denials |
| 2 | Charge Capture & Medical Coding | Assign ICD-10, CPT, and HCPCS codes for services provided to ensure accurate billing |
| 3 | Claim Submission | Create and electronically submit a formal claim to the payer or clearinghouse |
| 4 | Payer Adjudication | Insurance reviews the claim, applying their policies to approve, deny, or reject |
| 5 | Payment Posting | Log payments and adjustments in patient accounts for clear reconciliation |
| 6 | Accounts Receivable (A/R) Follow-Up | Track, investigate, and resolve any outstanding claims to maximize collections |
| 7 | Denial Management and Patient Billing | Correct denied claims and bill the patient for remaining balances to recover lost revenue |
Average Time Spent per Step
Each phase in the billing process takes time, and even small delays can slow down payments. Knowing how long each step usually takes helps a practice see where things get stuck and where improvements will have the biggest impact.
Billing Step | Avg Time Required |
|---|---|
| Pre-Authorization | 5–15 minutes per patient |
| Registration & Verification | 5–10 minutes |
| Coding & Charge Capture | 10–20 minutes |
| Claim Submission | 1–2 minutes |
| Payer Adjudication | 15–30 days |
| Payment Posting | 3–5 minutes |
| A/R Follow-Up | Weekly–monthly |
| Denial Management | 24–48 hours per claim |
| Patient Billing | 5–10 minutes per account |
According to the Medical Group Management Association, inefficient billing processes raise administrative costs by more than ten percent and push the payment cycle a number of weeks further back. Simple changes such as automation of verification, close tracking of claims, and set follow-up routines can significantly speed up reimbursements.

What Is a Clean Claim Rate?
A clean claim is a medical billing claim submitted without errors, missing information or compliance issues that would cause a payer to deny or delay it. The clean claim rate measures what percentage of your submitted claims are accepted and processed on the first submission without requiring correction or resubmission. Industry benchmarks from MGMA suggest that efficient practices maintain a clean claim rate above 95%. Practices falling below this threshold are typically losing revenue to front-end errors in coding, documentation or eligibility verification.
What is Prior Authorization in Medical Billing?
Prior authorization (PA) is a payer requirement that certain services be approved before they are delivered. Without PA when required, the claim is automatically denied regardless of medical necessity. Services commonly requiring prior authorization include specialty medications and biologics, elective surgical procedures, advanced imaging (MRI, CT, PET) and inpatient admissions.
Starting in 2026 under CMS-0057-F, Medicare Advantage, Medicaid managed care, and Marketplace plans must give fast prior authorization decisions within 72 hours and regular decisions within 7 days. Keeping track of PA rules for each payer and service is one of the best ways to protect your revenue in medical billing.
Types of Medical Billing Services
Practices can choose among three main models for managing their billing operations. The best fit depends on the practice’s size, specialty, and financial goals.
| Feature | In-House Billing | Outsourced Billing | Hybrid Billing |
|---|---|---|---|
| Control | Staff and processes are fully managed internally | Managed by external experts via a service agreement | Shared control. Internal team handles front-end; experts handle backend |
| Cost | High fixed costs from salaries, software, and training | Variable fee, often a percentage of collections | Moderate blend of fixed and variable costs |
| Expertise | Limited to knowledge of the in-house team | Access to certified specialists familiar with payer rules | Leverages both internal and external knowledge |
| Scalability | Difficult and expensive to scale | Scales quickly with practice volume | Moderately scalable |
| Technology | Requires investment and ongoing maintenance | Advanced software and analytics included | Mix of internal and vendor-provided tools |
| Best For | Large practices with dedicated resources | Practices seeking efficiency and cost reduction | Organizations wanting a tailored approach |
Why Outsource Medical Billing: Cost, Performance and Efficiency Comparison
Every healthcare practice invests time and money to get paid for the care it provides. But when billing is managed entirely in-house, that investment often grows faster than the return. Salaries, software subscriptions, ongoing coder training, compliance audits and IT maintenance add up quickly. Claim volumes fluctuate, denials rise and fall, payer rules change and staff availability varies.
Outsourcing changes the equation. Instead of carrying fixed costs, you pay for measurable performance. External billing specialists already have certified teams, advanced RCM software and established compliance systems. You access all of that instantly without building or maintaining it yourself. According to the Healthcare Financial Management Association’s Revenue Cycle Benchmarking Report, outsourcing medical billing cuts operational costs by up to 30% and shortens reimbursement cycles by 20 to 40%.
| Metric | In-House | Outsourced |
|---|---|---|
| First-pass clean claim rate | 80% | 98% |
| Average Days in AR | 45 | 30 |
| Cost as % of collections | 10 to 12% | 6 to 8% |
| Staff time on billing tasks | About 30% of admin hours | Less than 10% |
Cost of Inefficient Billing
Every claim error, missing document, or late submission chips away at a healthcare provider’s revenue. Billing inefficiencies are not just administrative setbacks; they directly affect profitability, compliance risk, and cash flow stability.
| Metric | Industry Insight | Source |
|---|---|---|
| Average claim denial rate | Roughly 30% of medical claims are denied or rejected on their first submission, representing billions in lost revenue each year. | MGMA |
| Claim rework cost per denial | Each denied claim costs an average of $25 to correct and resubmit, not including lost staff time or delayed reimbursements. | Change Healthcare 2023 Revenue Cycle Denials Index |
| Administrative cost of billing | Billing-related tasks consume up to 14% of a physician’s total revenue, mostly due to manual entry and repetitive processes. | JAMA |
| HIPAA violation fines | Non-compliance penalties can range from $100 to $50,000 per incident, with an annual maximum of $1.5 million. | HHS.gov |
| Impact of outsourcing billing | Practices that outsource to certified billing specialists see collection rates improve by 15–20% and denial rates drop by nearly half. | AAPC |
| Days in Accounts Receivable (A/R) | Industry benchmarks suggest that efficient billing systems maintain A/R below 40 days, while poorly managed systems average 60–90 days. | HFMA |
All these numbers show that billing inefficiency isn’t just about errors. It also means missing out on chances to grow revenue and keep your finances stable over time.
Key Challenges in Medical Billing
Each denied claim or delayed payment affects more than just the numbers. It leads to workflow problems, overworked staff, and lost time, all of which can hurt patient care and revenue.
To understand where these inefficiencies begin, it helps to look at the most common challenges that disrupt billing operations.
| Challenge | Operational Impact | Effective Solution |
|---|---|---|
| High Denial Rates | Each denied claim requires rework, slowing down payments and increasing administrative costs. | Automate claim scrubbing and track denial trends to address recurring issues. |
| Staff Turnover | High turnover disrupts workflows and increases training costs, leading to inconsistency in claim handling. | Standardize processes and use automation to reduce dependency on manual tasks. |
| Regulatory Complexity | Frequent updates to HIPAA and CMS guidelines make compliance management difficult. | Conduct quarterly audits and staff training to stay aligned with regulations. |
| Manual Workflows | Paper-based or fragmented systems increase error rates and slow reimbursement cycles. | Integrate EHR and RCM tools for faster, more accurate data transfer. |
| Evolving Payer Requirements | Constant changes in payer policies lead to confusion and inconsistent reimbursement. | Use payer portals and automated eligibility verification for real-time updates. |
Each of these challenges feeds into the next, creating a cycle of inefficiency that is difficult to break without structural improvement. Among them, one issue stands out as both the most frequent and the most preventable: claim denials.
Most Common Reasons for Claim Denials
When a payer denies a claim, they attach a Claim Adjustment Reason Code (CARC) that specifies why. Understanding these codes is the first step in fixing and resubmitting denied claims.
| Denial Code | Meaning | Common Cause |
|---|---|---|
| CO-50 | Not medically necessary | Diagnosis does not support the procedure |
| CO-16 | Missing or invalid information | Incomplete documentation |
| CO-4 | Incorrect procedure code | CPT or modifier mismatch |
| CO-97 | Service included in another procedure | Bundling or unbundling error |
| CO-29 | Timely filing limit exceeded | Late submission |
| PR-96 | Non-covered charge | Service excluded by payer |
Identifying patterns in your denial codes reveals systemic problems. If CO-50 is your top denial, the issue is medical necessity documentation. If CO-16 dominates, the issue is front-end eligibility and documentation collection. Fix the pattern, not the individual claim.
According to MGMA, up to 90% of denials are preventable through better front-end verification, coding accuracy, and real-time claim tracking. Understanding the leading causes helps providers take proactive action.
| Reason for Denial | Estimated Share | How to Prevent It |
|---|---|---|
| Incomplete patient information | 25% | Verify demographics and insurance details before each visit. |
| Coding errors | 22% | Conduct regular coding audits and ensure staff stay updated on ICD-10 and CPT revisions. |
| Insurance ineligibility | 20% | Use automated eligibility verification tools to confirm coverage at scheduling. |
| Late submission | 18% | Configure RCM software to flag claims approaching submission deadlines. |
| Other causes (authorization, duplicates, etc.) | 15% | Implement claim tracking dashboards for early error detection. |
Most claim denials start with front-end errors. Fixing the first few minutes of your billing workflow can save weeks of downstream rework.
Addressing these issues at the front end of the billing process is far more cost-effective than resolving them later. While no system can eliminate denials entirely, the right mix of automation, process design, and expert oversight like the approach used by Dastify Solutions, can significantly reduce their frequency and financial impact.
How to Read an Explanation of Benefits (EOB)
An EOB is a document sent by the payer after a claim is processed. It’s not a bill. It shows what was billed, what the payer paid, and what the patient still owes.
Key EOB sections to review:
- Billed amount: What the provider charged
- Allowed amount: What the payer’s contract allows
- Plan paid: What the insurance company actually paid
- Patient responsibility: Copay, deductible or coinsurance owed by the patient
- Adjustment reason: Why any difference exists between billed and allowed amount
When the EOB shows an allowed amount significantly lower than the billed amount, it may indicate a fee schedule discrepancy or a non-covered service. When it shows a denial, the CARC code in the adjustment reason section specifies the exact denial reason. Billing teams should review every EOB within 48 hours of receipt to catch underpayments before they age beyond appeal deadlines.
HIPAA Compliance in Medical Billing
The Health Insurance Portability and Accountability Act applies directly to medical billing operations in three ways:
| 1. Protected Health Information (PHI) | 2. Electronic Transactions | 3. Business Associate Agreements |
|---|---|---|
| Every claim contains patient PHI (name, diagnosis, procedure, insurance ID). Billing teams handling this data must follow HIPAA’s Privacy and Security Rules. | HIPAA mandates standard formats for electronic claims (X12 837P for professional claims, X12 837I for institutional), eligibility checks (270/271) and remittance advice (835 ERA). | Any billing company handling PHI must sign a BAA with the covered provider, establishing shared responsibility for data protection. |
HIPAA violation fines can range from $100 to $50,000 per violation, depending on the situation, with a yearly maximum of $1.5 million per violation type. If you outsource billing, you must make sure your billing partner has up-to-date HIPAA compliance certifications and a signed BAA. This isn’t optional, it’s required by law.
Medical Billing Technology Trends: AI, Automation and Predictive Analytics
Medical billing is becoming smarter and more connected. The focus is moving from just processing claims to using systems that spot problems early, keep providers updated, and help patients better understand their costs.
| 1. Predictive Tools That Prevent Errors | 2. Clear, Real-Time Reporting | 3. A Better Patient Experience |
|---|---|---|
| Modern billing platforms can now spot likely denials before a claim is sent. By analyzing past data and payer behavior, they help staff correct problems early. Studies from CAQH show that automation and predictive tools could save U.S. providers more than $16 billion a year by reducing rework and manual follow-ups. | Instead of waiting weeks for claim updates, practices are beginning to use dashboards that show revenue flow and claim status in real time. This visibility allows administrators to act quickly, track performance, and plan resources with confidence. | Patients now expect clarity. Digital billing portals, upfront cost estimates, and easier payment options are becoming standard. These tools build trust and reduce confusion about what patients owe and why. |
| 4. Connected and Cloud-Based Systems | 5. Smarter Compliance |
|---|---|
| Cloud billing platforms are replacing disconnected software. When billing tools work directly with electronic health records, information moves smoothly from visit to payment, cutting down on errors and delays. | Frequent updates from CMS and private payers make manual rule tracking impossible. Modern systems handle those updates automatically, helping practices stay compliant and avoid costly mistakes. |
Why Outsource your Billing to Dastify Solutions
Dastify Solutions combines technology, expertise, and compliance to help practices:
- Minimize billing errors by 99%
- Reduce AR turnaround by 40%
- Process 95% clean claims
- Increase revenue by up to 20%
Our experts manage the end-to-end billing process, allowing providers to focus on patient care.
To Sum It Up
Medical billing is not just a back-office function. It is the system that determines whether your practice gets paid for the work it does. When billing runs well, revenue flows, compliance stays intact and your team spends less time chasing denials and more time on patient care.
This guide covered the fundamentals. For specialty-specific billing complexity, Dastify handles oncology, orthopedics, cardiology, behavioral health, regenerative medicine, neonatology and 30+ other specialties with billing workflows built for each one.

Frequently Asked Questions
What are the steps in the medical billing process?
The process starts with patient registration and insurance verification, followed by coding, claim submission, payer review, payment posting, and denial follow-up. Each step ensures that providers are reimbursed accurately and on time.
What is the difference between medical billing and coding?
Coding turns medical procedures and diagnoses into standardized codes like ICD-10 and CPT. Billing uses those codes to create claims, submit them to insurers, and follow up until payment is received.
Why is accurate medical billing important?
Accurate billing prevents denials, reduces delays, and keeps revenue consistent. It also helps practices stay compliant with HIPAA and CMS rules while protecting patient data.
How does RCM improve healthcare finances?
Revenue Cycle Management (RCM) connects every financial step from scheduling to payment. Strong RCM systems reduce claim rework, shorten A/R days, and improve cash flow and collection rates.
What are the latest trends in medical billing technology?
Automation, predictive analytics, cloud-based billing, and AI-driven denial prevention are transforming billing accuracy and speed. Integrated EHR and RCM systems also give providers real-time visibility into their revenue.



