If you’ve ever felt frustrated by patients waiting days for treatments because of insurance approvals, you’re not alone. Do you know? 94% of U.S. physicians report that prior authorization delays patient care ; PA is no longer an admin headache, it’s a patient care risk. As PA requirements continue to increase and new CMS rules take effect in 2026, practices that rely on manual workflows are seeing longer delays, staff burnout, and growing revenue risk.
This guide shows how high-performing practices are using proven strategies to cut prior authorization time in half. From standardized workflows to AI-enabled tools, these methods streamline approvals, reduce denials, and protect patient care.
A Proven Workflow That Cuts Prior Authorization Time by 50%
Below is the step-by-step process used by high-performing physician practices and billing teams.
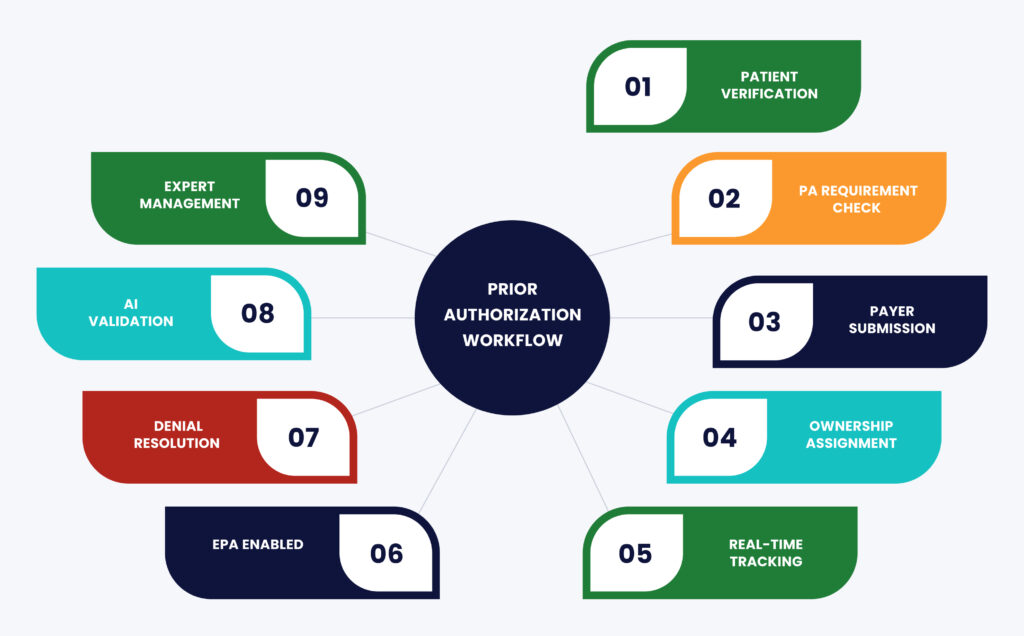
Step 1. Standardize Patient Intake
The fastest approvals start before the request is submitted. Ensure that your staff captures:
- Correct patient demographics
- Verified insurance coverage
- Accurate procedure and diagnosis codes
- Complete supporting documentation
Step 2: Confirm Prior Authorization Is Required
Not every service requires PA. Before submitting:
- Check payer-specific PA requirements
- Confirm service, location, and provider eligibility
- Avoid unnecessary submissions that waste time
Step 3: Follow Payer-Specific Submission Rules
Each payer has its own portals, forms, and documentation standards. Best practices:
- Maintain payer-specific PA checklists
- Use the correct submission method the first time
- Track payer turnaround timelines
“Submitting The Wrong Form or Portal Can Add Days To The Approval Process.”
Step 4: Assign Dedicated Authorization Ownership
When PA tasks are shared across staff, requests stall. High-efficiency practices:
- Assign dedicated staff (or billing partners) to PA
- Track each request from submission to decision
- Schedule follow-ups at defined intervals
Clear ownership alone can significantly reduce delays.
Step 5: Track Every Authorization in Real Time
Manual tracking leads to missed follow-ups. Effective PA tracking includes:
- Real-time status visibility
- Automated reminders for follow-ups
- Flags for stalled or overdue requests
This prevents approvals from sitting idle.
Step 6: Use Electronic Prior Authorization (ePA)
Electronic PA dramatically reduces turnaround time:
- Faster submissions
- Digital confirmation and audit trails
- Reduced phone calls and faxing
- Faster payer responses
Many practices see approvals in hours instead of days after switching to ePA.
Step 6a: Integrate FHIR API Workflows
Modern PA tools don’t just rely on portals; they use mandated FHIR-based APIs to query payer clinical criteria in real-time (CMS-0057-F). This allows your system to pre-validate documentation before submission, reducing errors and speeding approvals.
Step 7: Act Quickly on Denials
With new CMS rules, payers must provide specific reasons for denial.
Best practices:
- Address missing documentation immediately
- Correct coding issues quickly
- Resubmit without restarting the process to prevent delays in care and lost revenue.
Providers See AI as a Strategic Answer to Prior Authorization Inefficiencies 99% of clinicians report confidence in AI-assisted PA tools to reduce administrative burden.
Step 8: Use AI-Enabled Tools to Prevent Delays
Modern billing services use AI to:
- Identify PA requirements automatically
- Validate documentation completeness
- Predict denial risk
- Trigger follow-ups before deadlines are missed
Step 9: Outsource Prior Authorization to Billing Experts
For many practices, the fastest way to cut PA time is to partner with a medical billing service that manages prior authorizations end-to-end.
Billing specialists:
- Submit and track PAs daily
- Follow payer-specific rules
- Handle denials and resubmissions
- Free your staff from constant follow-ups.
Why Do Prior Authorizations Take So Long?
Prior authorizations take time because they rely on fragmented, manual processes that were never designed for today’s patient volumes.
Most delays occur due to:
- Incomplete patient or insurance information
- Missing clinical documentation
- Payer-specific submission rules
- Phone- and fax-based follow-ups
- No dedicated staff ownership
Physicians and their staff now spend an average of 12–13 hours per week on prior authorization paperwork, time that should be spent on patient care.
Prior Authorization Changes 2026 Physicians Must Know
New CMS rules and payer requirements are changing PA timelines, denials, and electronic approvals. Outsourcing reliable medical billing services can significantly reduce this burden.
| Meet Mandatory PA Timelines (CMS Rule) | Standardize Submissions & Go Electronic | Protect Continuity of Care | Move to ePA & FHIR API Workflows |
|---|---|---|---|
| Urgent Requests: 72 hours, Standard: 7 days Many practices struggle to track and meet deadlines. | Reduce unnecessary PAs, honor authorizations when patients switch plans, improve transparency. | New insurance plans must honor prior approvals for ongoing treatments (90-day transition). | Only 23% of physicians report that their EHR system offers electronic PA for prescription medications. Target: 80% of PAs electronically approved by 2027. |
Achieve Gold Carding Status
High-performing practices may qualify for Gold Carding, exempting them from future PA requirements. Our 98%+ first-pass approval rate positions your practice as a candidate, potentially eliminating future PA hurdles entirely.
Key PA & Billing Benchmarks for 2026 Success
Use this checklist to evaluate your practice or billing partner’s performance. These benchmarks reflect high-performing AI-enabled medical billing services
| Metric | Industry Benchmark |
|---|---|
| Billing Accuracy | 99% |
| A/R Reduction | 40% |
| First-Pass Clean Claim Rate | 98%+ |
| Revenue Increase | Up to 20% |
| Denial Rate | ≤4% |
| Turnaround Time | 7–14 Days |
Final Thought: Prior Authorization Shouldn’t Delay Care
Dastify Solutions helps U.S. physician practices by handling prior authorizations as part of our medical billing services from submission to approval, so your staff doesn’t spend hours on the phone, and your patients aren’t left waiting.



